Training in Modern Lower Extremity Revascularization: Analysis of the Operative Experience of Surgical Trainees over Twenty Years
Alexander H. Shannon, MD1, Bernadette J. Goudreau, MD1, Derek de Grijs, MD1, Ian Cook, BS1, Zachary M. Tyerman, MD1, J. Michael Cullen, MD1, Gilbert R. Upchurch, Jr., MD2, William P. Robinson, III, MD1.
1University of Virginia, Charlottesville, VA, USA, 2University of Florida, Gainesville, FL, USA.
Objectives: Lower extremity (LE) revascularization training has changed over the last 20 years, with increased emphasis on endovascular procedures and development of integrated programs. The impact of these changes on surgical resident LE revascularization experience is unclear. The objective of this study was to evaluate national trends in training in LE revascularization of general surgery residents (GSR), vascular fellows (VF), and integrated vascular residents (IVR) over the past 20 years. We hypothesized that GSR LE revascularizations are down trending and patterns among VF and IVR may further define these changes.
Methods: ACGME vascular surgery case logs were queried from 1999-2017. National GSR, VF, and IVR averages for each year were collected for the following case types: LE peripheral open cases, LE peripheral endovascular cases, and total overall LE vascular cases. Changes in operative volume over time were quantitatively analyzed using linear regression and comparison of best-fit line to a slope of zero (indicating no change).
Results: Average number of LE revascularization procedures performed by all surgical trainees increased from 1999-2017 (p < 0.0001). GSR demonstrate significant decrease in total LE cases (p = 0.0004), while VF experience increased (p = 0.0317). Average number of cases per IVR remained stable (p = 0.08) (Figure 1A-D). When comparing open vs. endovascular cases, GSR show significant downward trend in open LE cases in the most recent recorded year (21.4-15.8, p = 0.0002) with a stable number of endovascular cases (4.5-5.3, p= 0.0743). VF are upward trending in open (93.5-101.3, p = 0.0045) as well as endovascular cases (80.3-98.3, p = 0.0334). IVR do not demonstrate statistically significant differences in case volume when evaluating open (112.8-128.5, p= 0.124) vs. endovascular (90.1-107.7, p =0.0787) procedures.
Conclusion: GSR LE revascularization experience significantly declined, especially in open cases whereas endovascular volume remained stably low. VF demonstrated an upward trend in all cases and IVR experience remained stable in all areas. Strategic changes to the general surgery curriculum and vascular requirements may aid in providing a vascular experience to GSR that is more reflective of modern-day vascular practice. 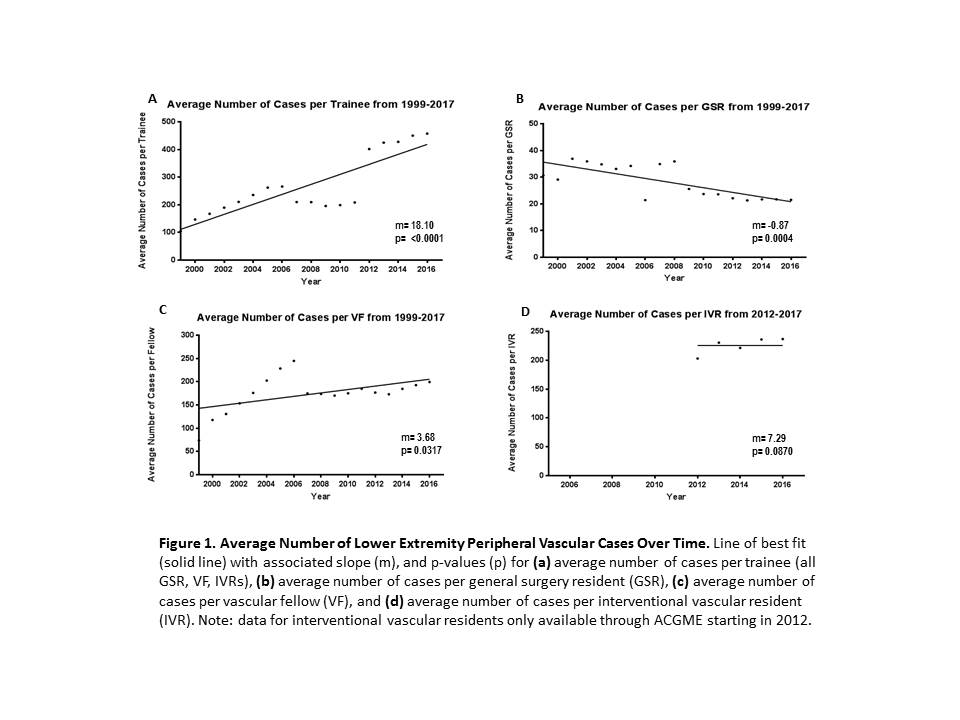
Back to 2019 Abstracts
