Outcomes and Predictors of Popliteal Artery Injury in Pediatric Trauma
Shelley Maithel, MD, Roy M. Fujitani, MD, Areg Grigorian, MD, Nii-Kabu Kabutey, MD, Sahil Gambhir, MD, Brian Sheehan, MD, Jeffry Nahmias, MD.
University of California, Irvine, Orange, CA, USA.
OBJECTIVES: Popliteal artery injury (PAI) is a rare occurrence in pediatric patients with significant consequences. Delays in diagnosis lead to severe complications such as life long disability and limb loss. We sought to identify outcomes and clinical predictors of PAI in the pediatric trauma population.
METHODS: The Pediatric Trauma Quality Improvement Program (2014-2016) was queried for patients < 17-years-old with PAI. Patient demographics and outcomes were characterized. A comparison of patients sustaining blunt versus penetrating PAI was performed. A multivariable logistic regression analysis was used to identify predictors of PAI.
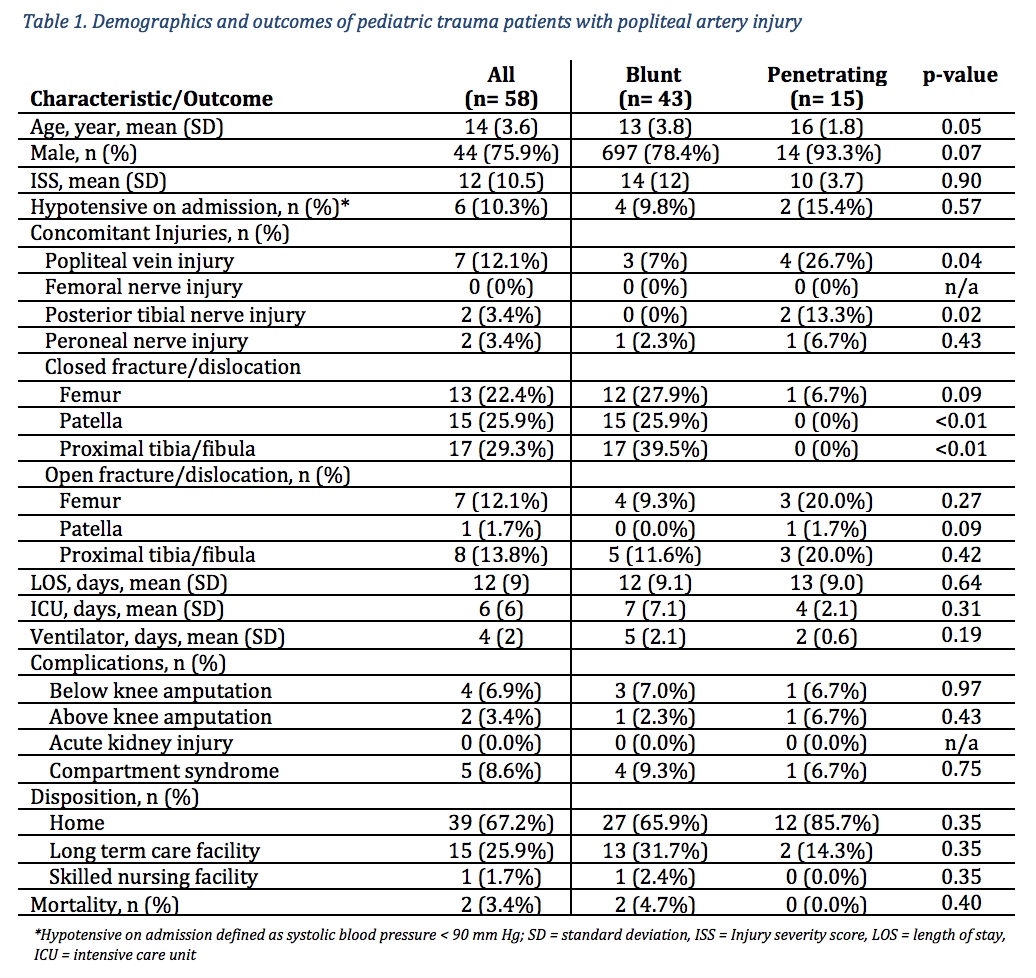
RESULTS: From 119,132 patients, 58 (<0.1%) sustained a PAI with 74.1% from blunt trauma. Most of the patients were male (75.9%) with a mean age of 14 and injury severity score of 12. Concomitant injuries included popliteal vein injury (PVI) (12.1%), posterior tibial nerve injury (3.4%), peroneal nerve injury (3.4%), and closed fracture/dislocation of the femur (22.4%), patella (25.9%), and tibia/fibula (29.3%). Patients with PAI secondary to penetrating trauma had a higher rate of concomitant PVI (26.7% vs. 7%, p=0.04) and posterior tibial nerve injury (13.3% vs. 0%, p=0.02) but a lower rate of closed fracture/dislocation of the patella (0% vs. 25.9%, p<0.01) and tibia/fibula (0% vs. 39.5%, p<0.01) compared to patients with PAI from blunt trauma. Overall complications included compartment syndrome (8.6%), below-knee amputation (6.9%), and above-knee amputation (3.4%). The overall mortality was 3.4%. After controlling for covariates, independent predictors for PAI included PVI (OR 296.57, CI=59.21-1485.47, p<0.001), closed patella fracture/dislocation (OR 50.0, CI=24.22-103.23, p<0.001), open femur fracture/dislocation (OR 9.05, CI=3.56-22.99, p<0.001), closed tibia/fibula fracture/dislocation (OR 7.44, CI=3.81-14.55, p<0.001), and open tibia/fibula fracture/dislocation (OR 4.57, CI=1.80-11.59, p<0.001). PVI had the highest association with PAI in penetrating trauma (OR 84.62, CI=13.22-541.70, p<0.001) while closed patella fracture/dislocation had the highest association in blunt trauma (OR 52.01, CI=24.50-110.31, p<0.001).
CONCLUSIONS: A higher index of suspicion should be present for PAI in pediatric trauma patients presenting with a closed patella fracture/dislocation after blunt trauma. PVI is most strongly associated with PAI in penetrating trauma. Prompt recognition of PAI is crucial as there is a greater than 10% amputation rate in the pediatric population.
$$graphic$$
Back to 2019 Abstracts
