Endovascular Salvage Of Chronically Occluded Femoral To Below Knee Popliteal Artery GSV Bypass With Gore Viabahn Relining
sai M. Kottapalli, DO, Richard Curl, MD, Linda Harris, MD.
University at Buffalo, Buffalo, NY, USA.
Demographics: 68 year old Caucasian male.
History: Past medical history of HTN, CAD, PAD s/p left femoral to below knee popliteal artery bypass with reversed greater saphenous vein (GSV) 6 months ago for disabling claudication. Improvement in pain free walking distance for 2 months post-op followed by recurrence of symptoms. Patient currently presents with rest pain and worsening leg swelling. Duplex study demonstrated occluded bypass with L ABI: 0.4. Given the findings on his recent cardiac cath, patient was unable to be cleared for any open surgical interventions.
Plan: Patient was cleared for a lower extremity angiogram with possible interventions. Multiple attempts were made to re-canalize the superficial femoral artery (SFA) and popliteal artery long segment occlusions. Unable to do so, we cannulated the bypass and relined the entire GSV conduit with 5x25cm X2 Gore Viabahn endoprosthesis (Fig 1). Patient was discharged home the same day on ASA + Xarelto 2.5mg BID. Seen post-op with complete resolution of rest pain and improved pain free walking distance.
Discussion: Patients with chronically occluded vein bypass and when unable to provide in-line flow to by re-canalization of occluded native vessels, relining of the occluded vein bypass with a covered stent is a viable option. Future studies are warranted to determine patency and limb salvage rates in individuals who undergo relining of occluded vein or prosthetic bypasses as an endovascular salvage of bypasses.
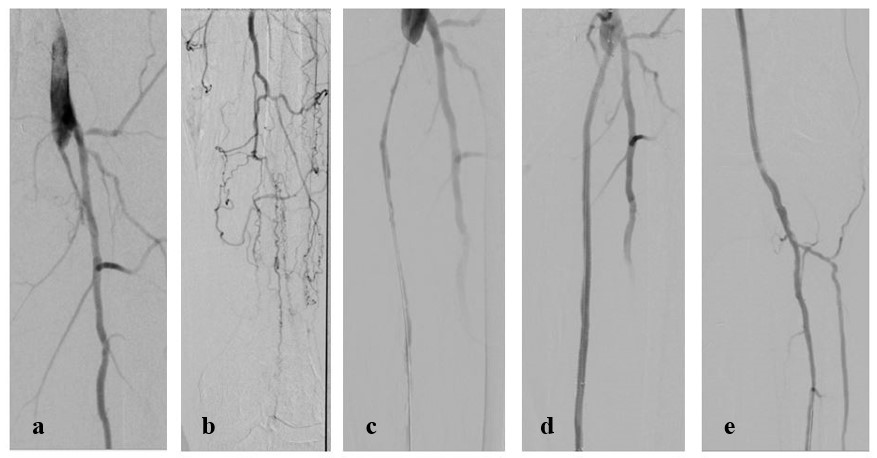
Fig 1: a) Occluded L superficial femoral artery. b) Occluded L femoral-below knee pop GSV bypass c) Re-canalization of occluded GSV conduit d) Viabahn relining of occluded GSV bypass e) In-line flow with 2 vessel runoff
Back to 2020 Abstracts
