Analysis Of Secondary Re-interventions For Persistent Endoleak After Initial Re-intervention
Christopher M. Faries, BA, Rami O. Tadros, MD, David Octeau, BA, Hanna J. Barnes, BA, Peter L. Faries, MD, Michael L. Marin, MD.
Icahn School of Medicine at Mount Sinai, New York, NY, USA.
Introduction: Persistent arterial perfusion of AAA after initial re-interventions (persistent endoleak) may require secondary reintervention (2 °RI). This study investigates the need for secondary re-intervention. Methods: A retrospective analysis of a prospectively maintained database was performed. From 1992-2019, 1638 patients underwent EVAR for AAA. 190 patients required re-intervention for endoleak. 61 of these required 2 °RI for endoleak. Durability was defined as freedom from reintervention for endoleak. Results: 136 patients required initial re-intervention for type I endoleaks, 15 for type III endoleaks, 38 for type II endoleaks, and 1 for a type IV endoleak (Table 1). Average duration of follow-up after initial re-intervention/2°RI was 33.4±38/31.7±37.4 months. Factors predictive of the need for initial re-intervention were AAA diameter upon first postoperative visit (p<0.001), intraoperative complications (p=0.003), and cardiac comorbidities (p=0.001) on multivariate analysis. Average time from EVAR procedure to initial re-intervention was 40.9±36.2 months, and average time from initial re-intervention to 2°RI was 23.3±30.3 months. Durability of index EVAR procedures was significantly greater than durability of initial re-intervention for endoleak (p<0.01). All 2°RI failures were due to type I endoleaks, including failure of 2 distal extensions (38.16 months), one proximal cuff (4.14 months), one distal extension and proximal cuff (25.8 months), one bifurcated device (13.1 months), and one embolization (26.5 months). 5 patients experienced initial re-intervention and 2°RI for different endoleak etiologies instead of persistent endoleaks. All-cause survival was significantly greater in patients that received re-intervention for endoleak compared to patients who had EVAR but did not require re-intervention (p<0.01). All-cause survival was significantly lower in patients who received multiple re-interventions for endoleak compared to patients who had EVAR but no re-intervention (p<0.01). Conclusion: AAA diameter, intraoperative complications and cardiac comorbidities were associated the need for initial re-intervention. Re-interventions for endoleak appear to be less durable than EVAR. While re-intervention for endoleak is associated with increased survival, 2°RI for endoleak is associated with decreased survival. Failure of 2°RI is seen in some cases following type I endoleaks. 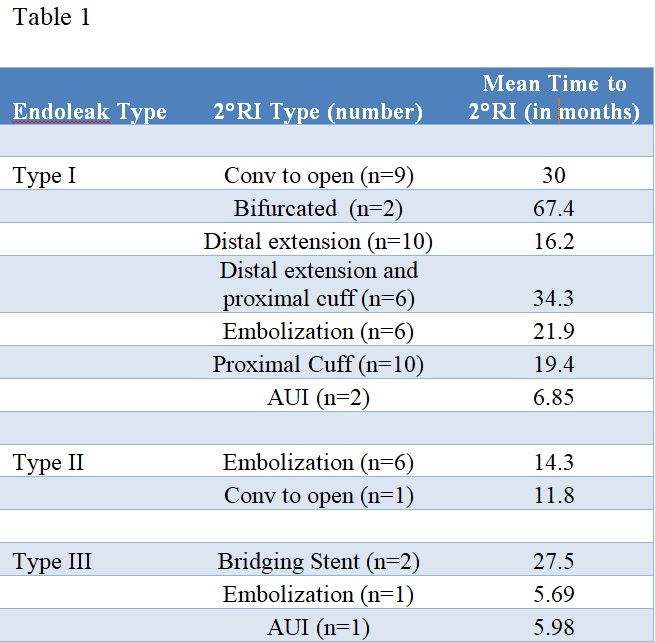
Back to 2021 Abstracts
