The Natural History Of Penetrating Atherosclerotic Ulcers In Aortic Branch Vessels
Charles DeCarlo, MD, Christopher A. Latz, MD MPH, Laura T. Boitano, MD MPH, Harold D. Waller, MD, Brandon Sumpio, MD, Anna A. Pendleton, MD, Samuel I. Schwartz, MD, Anahita Dua, MBChB, MBA, MSc.
Massachusetts General Hospital, Boston, MA, USA.
Objective - Penetrating atherosclerotic ulcers (PAU) in aortic branch vessels are rare. There is a paucity of data regarding their natural history in long-term follow up. This study determined the prevalence and natural history of aortic branch PAU.
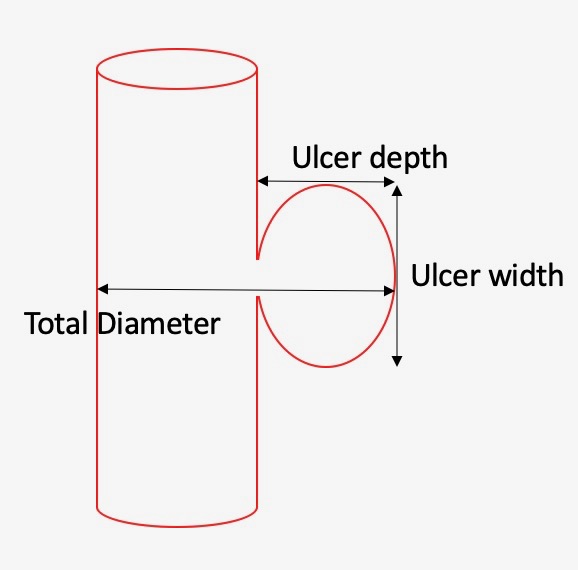
Methods - Institutional data on all patients with an aortic branch PAU 2005-2020 were gathered. Branch PAUs were defined as any PAU in the iliac, mesenteric, or arch vessels. Endpoints included symptoms, end-organ events, and interventions. Total diameter, ulcer width, and ulcer depth (Figure) were recorded on each CT scan for the branch PAU’s and rate of change was compared between groups (iliac vs. arch and visceral vessels) using linear mixed effects model.
Results - Among 58,800 patients who underwent a CTA, 433 patients had an aortic PAU (prevalence: 0.7%) and 58 patients had a branch PAU (prevalence: 0.1%). Among those 58 patients, there were 66 ulcerated branches. There were 50 iliac (42 common iliac, 7 internal, and 1 external), 11 arch (8 left subclavian, 3 innominate), and 5 visceral ulcers (3 SMA, 1 celiac, and 1 renal). Mean age was 74.0±8.8 years, 86% of patients were male, 74% had hypertension, 79% had hyperlipidemia and 59% had a concomitant aortic aneurysm. There were 45 PAU vessels with >1 CTA (total of 167 CTAs) with a median follow-up of 4.0 years [IQR:2.0-6.2]. Total vessel diameter increased in size by 0.27 mm/year but did not differ between groups (iliac vs. visceral/arch vessels). PAU width and depth also did not significantly change over time, nor did it differ between groups (Table). No branch PAUs caused symptoms, end-organ events, rupture, nor required intervention due to symptoms and/or progression. Four PAU spontaneously resolved (2 iliac, 2 other) and 1 iliac PAU progressed to saccular aneurysm.
Conclusions - Branch PAU’s are rare with a 0.1% prevalence. There was minimal growth noted in a median follow-up of four years and no PAUs required intervention for symptoms or progression. Asymptomatic branch PAUs may be safely observed.
| Table: Ulcer Size and Change in Size for PAU with >1 CT Scans | |||
| Iliac | Other Branches | p-value | |
| N=36 | N=9 | ||
| Initial Ulcer Width (mm), mean (SD) | 7.0 (5.0) | 4.7 (2.2) | 0.18 |
| Initial Ulcer Depth (mm), mean (SD) | 7.6 (2.6) | 5.1 (2.1) | 0.010 |
| Initial Total Vessel Diameter (mm), mean (SD) | 17.3 (5.0) | 14.6 (3.6) | 0.13 |
| Ulcer Width Change per Year (mm/year) | 0.04 | 0.12 | 0.801 |
| Ulcer Depth Change per Year (mm/year) | 0.05 | -0.09 | 0.42 |
| Total Vessel Diameter Change per Year (mm/year) | 0.27 | 0.32 | 0.831 |
| mm=millimeters | |||
Back to 2021 Abstracts
