Outcomes Of Chimney/Snorkel Endovascular Repair For Symptomatic And Ruptured Abdominal Aortic Aneurysms
Eric G. Jernigan, MD, Allen M. Conway, MD, Nhan Nguyen Tran, Khalil Qato, MD, Gary Giangola, MD, Alfio Carroccio, MD.
Lenox Hill Hospital, Northwell Health, New York, NY, USA.
OBJECTIVES: Symptomatic and ruptured abdominal aortic aneurysms (AAA) are increasingly managed with endovascular aneurysm repair (EVAR). We aimed to identify the 30-day outcomes of symptomatic and ruptured AAAs that underwent EVAR with chimney or snorkel techniques (Ch-EVAR).METHODS: A retrospective cohort study was performed using the Vascular Quality Initiative registry from March 2013-July 2019. All patients with symptomatic and ruptured AAAs with proximal aortic zone of disease from 6-9, who underwent Ch-EVAR were included. Outcomes were analyzed per the Society for Vascular Surgery reporting standards for EVAR.RESULTS: Ch-EVAR was performed in 77 patients (35 [45.5%] ruptures, 42 [54.5%] symptomatic). Median age was 73 (IQR, 67-81) years, and 54 (70.1%) patients were male. Maximum aneurysm diameter was 67.5 (IQR, 54.5-83.3) mm. All patients were ASA Class 3 or above, with 56 (72.7%) Class 4. Among ruptured AAAs, the mean lowest pre-operative SBP was 95.3 (±29.3) mmHg. Fluoroscopy time was 57.4 (IQR, 41.2-79.0) minutes. The proximal aortic zone of disease was zone 6 in 9 (11.7%), zone 7 in 21 (27.3%), zone 8 in 36 (46.8%), and zone 9 in 11 (14.3%) patients. Ch-EVAR involved 1 vessel in 28 (36.4%) patients, 2 vessels in 22 (9.1%) patients, 3 vessels in 19 (24.7%) patients, and 4 vessels in 8 (10.4%) patients. Technical success was achieved in 67 (87.0%) patients. Outcomes comparing symptomatic versus ruptured Ch-EVAR are summarized in Table I. Re-intervention was required in 10 (13.0%) patients at a median time of 9 post-operative days. This involved the aorta/chimneys in 5 (6.5%) patients, access ischemia in 1 (1.3%), complete device removal in 1 (1.3%), new stent placement in 2 (2.6%), and glue repair of endoleak in 1 (1.3%) patient. Postoperatively, 31 (40.3%) patients had a major complication, including 4 (5.2%) access site hematomas, 1 (1.3%) access site occlusion, 2 (2.6%) strokes, 2 (2.6%) pneumonias, 5 (6.5%) re-intubations, 8 (10.4%) renal ischemia, 11 (14.3%) post-operative dialysis, 4 (5.2%) intestinal ischemia, 3 (3.9%) leg ischemia, and 1 (1.3%) leg compartment syndrome.CONCLUSIONS: Ch-EVAR for symptomatic and ruptured AAAs may be performed with acceptable rates of morbidity and mortality. Long-term data are needed to determine durability. 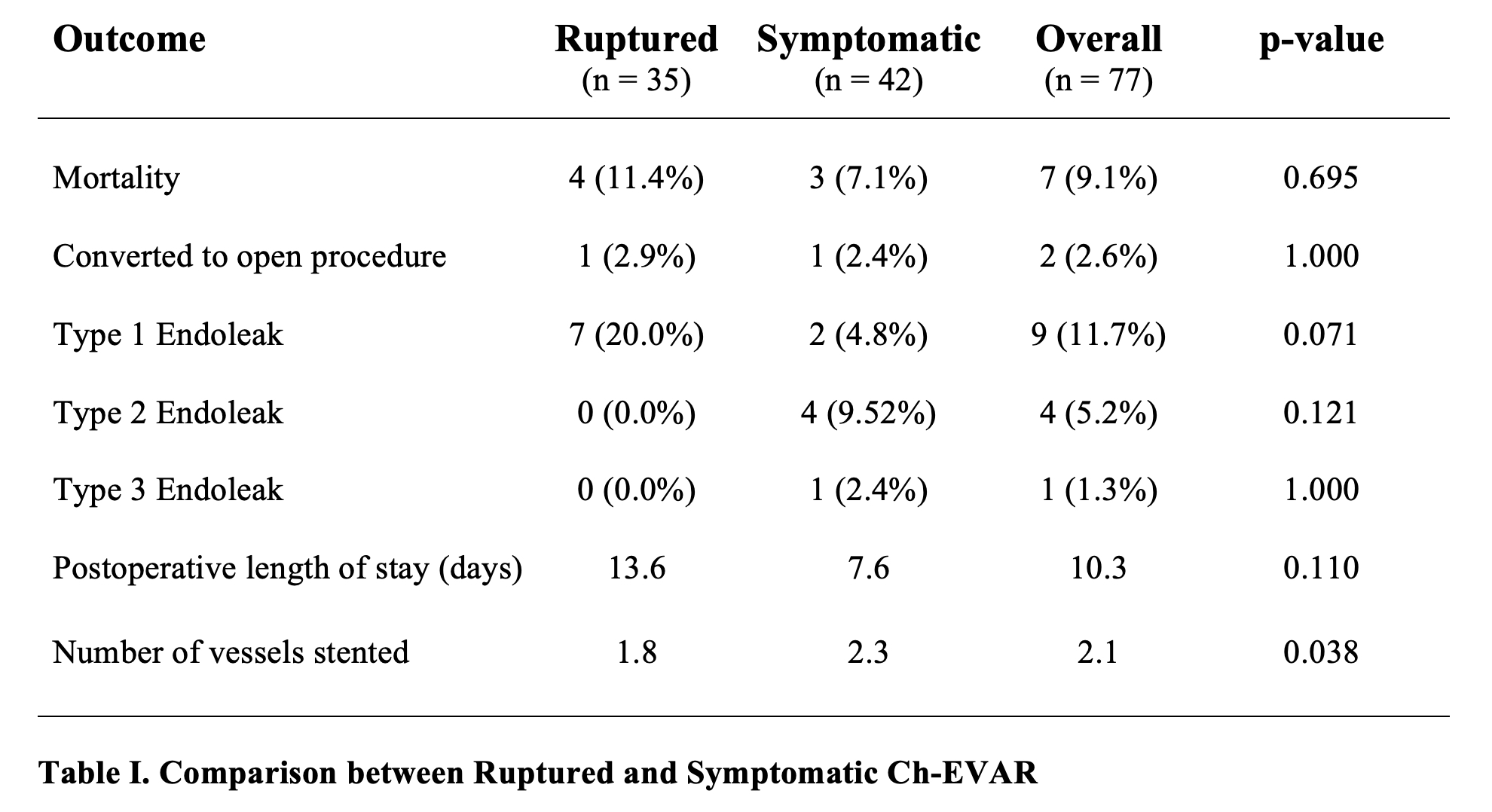
Back to 2021 ePosters
