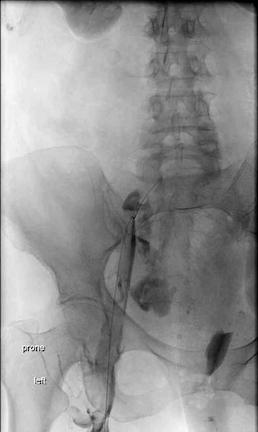
DEMOGRAPHICS: A 72-year-old caucasian female with a history of hypertension and hyperlipidemia and left total knee arthroplasty one month prior to presentation. HISTORY: She presented with shortness of breath, left lower extremity (LLE) swelling, and a syncopal event after walking outdoors. Blood pressure and heart rate were 75/55 and 128. She had a palpable left femoral pulse and a monophasic left posterior tibial signal. Her LLE was notably swollen with bluish discoloration and diminished sensation. CT angiogram of the chest, abdomen, and pelvis demonstrated subsegmental pulmonary emboli and moderate left retroperitoneal hemorrhage. LLE venous duplex demonstrated extensive thrombosis of the deep and superficial systems. PLAN: She was taken to the operating room for mechanical thrombectomy and evaluation of retroperitoneal hemorrhage. The left popliteal vein was accessed and a 5-french sheath was placed. A venogram demonstrated extensive iliofemoral DVT with extravasation of contrast from the common iliac vein. Intravascular ultrasound was performed. The sheath was upsized and a mechanical thrombectomy was performed with the Penumbra Lightning Flash device. An 18mm bell bottom Gore Excluder limb was removed from the delivery system, reversed, and deployed at the iliocaval confluence covering the common iliac tear. An additional 18 mm Gore Excluder limb was removed from the delivery system and deployed in the external iliac vein. Residual thrombus in the IVC was removed. Completion venogram showed excellent flow through the femoral vein into the IVC without extravasation.
DISCUSSION: Spontaneous common iliac vein rupture is an uncommon presentation of extensive iliofemoral DVT and has a high mortality rate. Predisposing events are frequently commonplace activities such as walking, defecating, and bending at the waist. There is an association with May-Thurner syndrome, and the vast majority of reported cases are in females and left-sided. Clinical manifestations included acute-onset left-sided abdominal or lumbar pain, lower extremity swelling and discoloration, acute anemia, and hypotension. Prior to the development of endovascular therapy, an open approach was utilized with direct repair, ligation, or bypass of the affected iliac vein and was associated with high morbidity and mortality. Recently, endovascular approaches have been utilized, including endovascular thrombectomy, IVC filter placement, and stent deployment.