Adherence to Lipid Management Guidelines and Outcomes in Patients Undergoing Revascularization for Chronic Limb-Threatening Ischemia
Thomas Fx O'Donnell, MD, Sarah E. Deery, MD, Jeremy D. Darling, Katie E. Shean, MD, Murray A. Mittleman, MD, Gabrielle N. Yee, Matthew R. Dernbach, Marc L. Schermerhorn, MD.
Beth Israel Deaconess Medical Center, Boston, MA, USA.
OBJECTIVES: The 2013 ACC/AHA Updated Practice Guidelines recommend the use of high dose statins in all patients <75y with chronic limb-threatening ischemia (CLTI), and moderate dose statins in CLTI patients >75y without contraindications or on hemodialysis, but these recommendations are based primarily on stroke and coronary data.1 We aimed to validate these guidelines in patients with CLTI and assess current adherence to these recommendations.
METHODS: We identified all patients with CLTI who underwent first time revascularization (endovascular or open) at a single institution from 2005 to 2014. Patients were classified as high dose, moderate, low or no statin postoperatively based on ACC/AHA guidelines. Major Adverse Limb Event (MALE)-free survival (death, amputation or major reintervention), overall survival, and amputations were recorded. Cox regression was used to account for differences in baseline characteristics.
RESULTS: After excluding patients on hemodialysis, we identified 1,033 limbs from 945 patients with a median followup of 380 days. Patients on recommended doses had higher rates of preoperative statin use, coronary artery disease, chronic kidney disease, stroke, atrial fibrillation, congestive heart failure and coronary artery bypass grafting, lower smoking rates and were less likely to be ambulatory preoperatively (all p<0.05). Overall, only 35% were on the recommended statin dosage; 55% of those above the age of 75 were on a moderate dose and 20% of those below 75 were on a high dose. In univariate analysis, patients on the recommended doses had lower rates of survival (P = .01), but no difference in rates of amputation, MALE-free survival, or RAS (all P > .05). After adjusting for confounders, cox regression demonstrated a 23% increase in the rate of MALE-free survival for patients on recommended doses (HR 0.77 [95% confidence interval 0.61-0.97], P = 0.03). Both subgroups of patients (>75 on moderate dose and <75 on high dose) accrued similar benefit from compliance with guidelines.
CONCLUSIONS: Compliance with recent guidelines is associated with significantly decreased limb events or death in patients undergoing revascularization for CLTI. Although adherence is increasing, two thirds of eligible patients are not on recommended doses, a potential target for improvement. 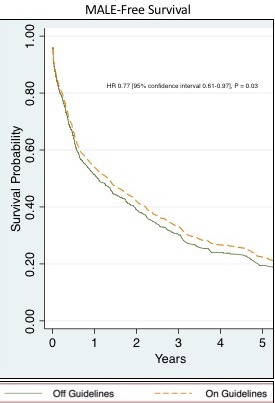
Back to 2017 Program




